Introduction
For being the pre-Columbian tobacco harm reduction technique, hookah (shisha, narghile, etc.) smoking had not posed any particular health problem for centuries, as acknowledged by world renowned tobacco and cancer researchers before year 2002 [49] . It suddenly began to “pose problems” (health?, social?, cultural?, political?, economical?) after that year. The question
“Why only after year 2002?”has been addressed in previous peer-reviewed publications (e.g.here) and in a SciTopic .A hookah (shisha, narghile, goza, etc.) is not a ““waterpipe”” (particularly in one word). This neologism proved to be a spurious scientific nominalism [14] . Most recent scientific evidence of its fatal consequences is exemplified by a recent cancer study in Egypt [20] ). Unsurprisingly, a bibliometric (“scientometric”) analysis found that this term was “over-represented” in the public health literature [3] . A hookah is a pipe that filters tobacco smoke (not only through water but as whole system) or, as it is more and more frequent these days, the one produced by heating a tobacco (or no-tobacco)-molasses and fruit based mixture in a bowl. The nature of the smoked products have changed to a certain extent: from raw plain tobacco (tumbâk, tumbeki, tütün) or jurâk (raw tobacco mixed with molasses [a sugar by-product] and/or soaked fruits, oils…) towards tobamel/moassel (mu‘assel in Arabic [i.e. a honeyed mixture]; “mel” meaning honey in Latin).The question of which word to use is very important and the answer is very simple. Let us use, depending on the social and human context, the words peoples have been using for centuries. The three main ones are: hookah (from Arabic huqqa = vase/recipient, i.e.the base of the pipe); narghile (form Sanskrit and Persian for coconut,i.e.used as a water container)[note that nargile is the Turkish spelling]; and shisha (from Persian “shishe”= bottle/recipient).
Society and Culture
Through centuries, the corresponding practice has created a whole culture based on a peculiar form of sociability that young people in the English-speaking world sometimes term “social smoking”. Indeed, this conviviality (from Latin “convivialis”= related to sharing [a meal, etc.]) deeply stamped many societies of Africa and Asia. This “bel objet” [nice to look at artefact] is often seen as: a pretext for conversation; a socially, religiously and sexually egalitarian, playful, libertarian, situationist and poetic symbol of time passing; not to mention a “peace pipe” etc. [6] .
Early medical anthropology research showed that children do not smoke the hookah and that women (particularly in Asia and Africa) are not accountable for the hookah epidemic, contrary to repeated statements by “”waterpipe”” experts [21] . As for the reasons behind the recent sudden world emergence of hookah smoking, up to 15 reasons were identified and published in key documents [6][7] . It is also noteworthy that the socio-cultural guard-rails (ritual, etiquette, etc.) were dissolved to a large extent as a result of the transplantation of the practice from its homelands to other continents (ibid.).
The Pre-Columbian Origins of the Hookah
The origins of the hookah go back far before the spread of tobacco across the world (16 th –17 th centuries). Contrary to international experts’ statements, the hookah is not of Indian origin. Its history is very complex and the main lines of the latter were set out in a comprehensive publication [6] . This document identified an early archaeological work showing that the most ancient traces were found in Southern or Eastern Africa. For instance, bowls of water pipes were dug out in 1971 by J.C. Dombrowski in the Lalibela cave (Ethiopia). Carbone 14 datation established that their use go back to around 1320 +/- 80A.D. [6][8] Then we have Shirazi’s poem (heralding the Knol on Irani women ), the first one in history about hookah (qalyan) smoking. It was written in 1535 so it is also very likely the first poem in the world about tobacco smoking. The related context was studied in detail in two books [6][25] .
As one can see, this date precedes Christopher Columbus’ travel to America and the consequent tobacco habits brought to Europe a few years later and disseminated all over the world. Historical accounts show that the large scale emergence of hookah in society, either for an individual or collective use, occurrred simultaneously with that of public coffee-houses and the adoption of tobacco in the Middle East region : near the end of the 16 th century and the beginning of the 17 th century [25].
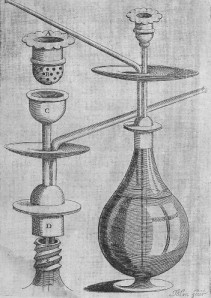
[picture: Persian qalyan. 17th century.The first human representation of a hookah. Souce: our book[6]]
History of Research on Hookah Smoking
Research on hookah did not start off in 2002 as “”waterpipe”” funding-hunting experts recently and publicy stated [10] . There had been numerous valuable scientific independent (this is very important) studies published over the last decades although, if a date were needed, it would be 1622 [6] . Because of their negative results, they have been systematically glossed over in present-day mainstream (antismoking) literature. Transdisciplinary (biomedical and social science) reviews of what research says about hookah smoking have been published over the last ten years and are still ongoing as exemplified by the first aetiologic study on hookah smoking and cancer ever published [9] . Focussing on the “water filter” is definitely a wrong approach to the problem. If it were so, then one should in fact consider six filters of varying efficiency, not only one: 1) the bowl where peculiar chemical reactions, very different from those induced by other tobacco use modes, occur ; 2) the vertical stem; 3) the water; 4) the suction hose; 5) the smoker’ lungs; 6) the socio-anthropological filter. Over the past centuries, the latter has definitively been the most powerful [6][14] .
One main problem in research published since 2002 is “parroting”, i.e., the pathetic trend among antismoking researchers to uncritically cite articles that previsouly appeared in the so-called “peer-reviewed” literature, sometimes without even reading them. This situation has resulted in the universal dissemination of serious scientific errors such as false statements about lung cancer, bladder cancer, etc. These errors have been “carried over” because they had been originally published by””waterpipe”” antismoking experts in the so-called “peer-reviewed” biomedical press. The most famous case is the following paper published in the main antismoking journal of the world : Maziak W, Ward KD, Afifi Soweid RA, Eissenberg T. Tobacco smoking using a waterpipe: a re-emerging strain in a global epidemic. Tobacco Control 2004; 13: 327-333.In spite of its numerous serious errors, the above article (which should be retracted from “Tobacco Control” if the latter were a responsible non-biased and truly peer-reviewed journal) served as the basis for the WHO (World Health Organisation) flawed report [21] and its recycled version, the similarly erroneous Cochrane review [28] . This is no surprise since their authors are the same in all cases…The draft of a list of about 300 hundred errorspublished so far in the peer-reviewed biomedical literature has been prepared in the form of a Knol:Anthology of serious errors
A Form of Officialised Revisionism in Biomedical Research
In 2010, an antismoking team (Elie Akl et al) from the University of Buffalo at New York has published a series of so–called “”systematic reviews”” on “”waterpipe”” smoking (health effects, lung function, survey instruments). [52][53][54] . These articles contain numerous errors and are stained by their striking publication bias (brushing aside independent studies with “negative” results in particular) “skewed toward” the bibliographical references of their antismoking colleagues of the US-Syrian and US-Lebanese antismoking centres [55][56] . They aim at setting the framework of “acceptable” research, i.e. research sticking to the political agenda of smoking Prohibition (FCTC, Globalink, etc.). This unacceptable attitude appears to be a form of officialised revisionism in biomedical research.
Thermodynamics, Physics and Chemistry of Hookah Smoking
The tobamel (moassel: tobacco (or tobacco-free)-molasses smoking mixture) is the most widely used product in Europe and the USA. It is actually a “light” and gooey version of the jurâk. It also contains glycerol which acts as a moistening agent and quite often flowers or fruits essences (apple, strawberry, rose, etc.). Once it is packed inside the bowl of the pipe, it must be covered with an aluminium foil perforated with small holes, that will be topped in its turn by one or several pieces of charcoal. The hot gases of their combustion, and not that of tobacco (as in cigarettes), will cause the “distillation” of some of its components (flavours, nicotine, etc.) [6][11] . Today the use of opium or cannabis remains very limited.
Tar is a complex set of chemicals, some of them (nitrosamines, polycyclic aromatic hydrocarbons) being extremely toxic. Hookah smoking (including with tobacco-free tobamel) produces tar. However, it is very different from that produced by cigarettes because of the great differences in temperatures: hundreds of degrees, which, from a chemical viewpoint, is of utmost importance. Notably, and in striking contrast with ordinary cigarettes, a great part of the aerosol in modern hookah is made up of dihydrogen monoxide [DHMO] and glycerol [4][9]
.Undoubtedly, these last chemical compounds, and particularly DHMO [13][35] (video) arehighly hazardous for human beings(*)and public health campaigns have emphasised this point. Consequently, calculating and advertising cigarette-equivalents of hookah smoking sessions makes no sense, particularly when “smoking machines”(drawing one puff every 17s over a full hour with the charcoal over the same position atop the bowl)are used for this purpose [9][15] .Indeed, a smoking machine, as that designed for the WHO (objective: world prohibition agenda through the implementation of the so-called ” Framework Convention on Tobacco Control ” – see elsewhere cogent critique of FCTC ) at the US-American University of Beirut, is a caricature of real natural human smoking. Hookah smokers are not robots [15] .Carbon monoxide (CO) -as well as other toxic substances such as polycyclic aromatic hydrocarbons- are mainly produced by the charcoal used to heat the smoking mixture [12][29] .Inhaled CO levels vary a lot and may reach those of pack-a-day cigarette smokers, particularly in ill-ventilated atmospheres [5][7][11][30][38] . CO is a very dangerous gas. Common symptoms of its action are headaches, pulse acceleration and muscular weakness. This is because CO prevents oxygen from binding to red blood cells and inside muscles [11] .CO poisoning due to hookah smoking has been reported in Turkey, Singapore and France. Fortunately, it is rather rare and when it happens here and there, it is due to the absence of efficient ventilation where hookah, generally with cigarette, smoking is performed [30] .
As for aldehydes (molecules that are quite aggressive to the respiratory mucous membranes), there is presently some confusion further to an experiment based on a biased smoking machine [16] . A critique of the latter has been published [15] . Even if the high levels of sugars in the smoking mixtures currently in use would be of concern (independent and objective studies are needed), there would be a solution (that will be detailed in a further version of this Knol).
(*) Note (onwhat was initially an ironical statementabout DHMOand glycerol): The following paragraph is an unreviewed anonymous “suggestion” (see ref. in right column) received on 2 Jul 2010:“Chemist here. Just wanted to let you know that DHMO, Dihydrogen Monoxide, is H20, which is Water. The DHMO cites you references are part of this hoax http://en.wikipedia.org/wiki/Dihydrogen_monoxide_hoax . I recognize that I’m citing wikipedia here, but I almost laughed out loud when I read the line about DHMO being dangerous. Glycerin is also not harmful and is frequently found in food products, it is metabolized safely by the liver. Best wishes.” See other comments from readers right at the end.
Hookah and Health (Diseases)
 As previouly said, hookah smoking had not posed any particular medical problem for centuries. However, it may today introduce new concerns because some of its inner anthropological characteristics, early documented but unfortunately censored, have been actually changing over the last two decades. For example, the nature of the smoked products changed or switched, as earlier said in the introduction: from raw plain tobacco of the tumbâk or jurâk types, both used within relatively standardised socio-cultural frameworks, towards tobamel/moassel. Amazingly, the latter produces a non-irritating smoke, much milder than that of a cigarette. This is, in part, because most of the irritants are watered down. Anyway, what is is noteworthy is that hookah users can inhale such a smoke directly into their lungs and, quite visibly, in great volumes.This has led to the following scientific misconduct on behalf ofhealth scares experts: equating the toxicity of such smoke with that of cigarettes. Obviously and fortunately, both smokes are completely different from all viewpoints(see, for instance, the above discussion about glycerol and DHMO). Please also refer to the above section for possible CO poisoning.
As previouly said, hookah smoking had not posed any particular medical problem for centuries. However, it may today introduce new concerns because some of its inner anthropological characteristics, early documented but unfortunately censored, have been actually changing over the last two decades. For example, the nature of the smoked products changed or switched, as earlier said in the introduction: from raw plain tobacco of the tumbâk or jurâk types, both used within relatively standardised socio-cultural frameworks, towards tobamel/moassel. Amazingly, the latter produces a non-irritating smoke, much milder than that of a cigarette. This is, in part, because most of the irritants are watered down. Anyway, what is is noteworthy is that hookah users can inhale such a smoke directly into their lungs and, quite visibly, in great volumes.This has led to the following scientific misconduct on behalf ofhealth scares experts: equating the toxicity of such smoke with that of cigarettes. Obviously and fortunately, both smokes are completely different from all viewpoints(see, for instance, the above discussion about glycerol and DHMO). Please also refer to the above section for possible CO poisoning.
However, hookah smoke (with moassel) is not pure oxygen. Its users should be aware that in the long term and in the case of heavy use, diseases comparable to those induced by cigarettes -particularly COPD (Chronic Obstructive Pulmonary Disease)- have been reported in the biomedical literature by independent (from the pharmaceutical industry) experts in Asia and Africa [6][11] . Other potential, but not documented, risks include infarction and arteritis. As for communicable diseases, and further to the related errors contained in the WHO flawed report on ““waterpipe”” smokingand blindly cited in The Lancet, [17] a clarification has now been published [12][19] .
Recently in Iran, a prestigious independent (from both the pharmaceutical and tobacco industries) team of researchers has found that cigarette and qalyân (one of the main two main forms of local water pipes) smoking are associated with
Nitric Oxide (NO) overproduction. As objective scientists, they warn (without being moralistic or fear arousing as their US antismoking counterparts) that NO overproduction can lead to pathological changes [51] . The same attitude is unfortunately not the same in a recent heavily biased antismoking study on the potentially genotoxic effects of hookah smoke [57] .
Concerning cancer, although the oral cancer hypothesis is acceptable, there is no need to hype unsusbtantiated claims about bladder, pancreas or lung cancer. Antismoking researchers have been clinging to the only study (among two dozens of other peer-reviewed publications pointing to the observed weak (or absence of) link) that would have found an association: Nafae et al [44] . In order to clear up meant confusion on behalf of antismoking researchers (particularly Cecile Ray with funding from “Physicians for Smoke-free Canada”; and a team of the US funded Syrian Centre for Tobacco Studies) [45][46][48] , a short critique of Nafae et al’s study was published in the British Dental Journal [32] . Then, recent clarifications appeared in other medical journals such as Medical Hypotheses and the International Journal of Cancer [49][50] (see also the ethical aspects of this campaign in a related knol). See also the related Knol about a “Systematic Review” (on cancer studies in particular) by Elie Akl et al. (University of New York at Buffalo),published in the International Journal of Epidemiology.
The first ever published two-fold aetiological study on hookah smoking and cancer led by Pakistani doctors (on rigorously selected exclusive hookah smokers who have been using, for decades and in several daily sessions, large amounts of tobacco;
the weight equivalent of up to 60 cigarettes in the bowl), show that overall CEA (CarcinoEmbryonic Antigen)[a biological marker for cancer] levels in that group were much lower (taking into account, in particular, the impressive amount of consumed tobacco) compared to those recorded among cigarette smokers. However, heavy hookah smoking substantially raises CEA levels [9] . For obvious reasons, these results have been swept under carpet (a common practice in ““waterpipe”” research) or their importance downplayed. For example, in a recent “review” full of errors (see relatedKnol on Cobb et al.), the authors ofthe WHO flawed report on ““waterpipe”” smokinghave actually cited our study on hookah smoking and cancer (probably under “peer-review” pressure or just to save their face) [40] . Amazingly, they selected the findings related to heavy smokers and discarded those about medium and light smokers. This choice was even more irrelevant that the two latter’s profiles are much more akin to those of the US-American users of the modern hookah.To close this section, it should be mentioned that a team of independent experts from Africa has recently reviewed in depth the claims widely published in the biomedical literature over the past years. Its conclusion is that it is necessary to clear up the worldwide growing confusion [33][34] . We believe that it has reached the highest levels in the history of tobacco research and the WHO has endorsed it. On recent developments (particularly a salvo of new publications during summer 2010), see Knol titled Narghilistan. Finally, another source of the confusion is that in many studies involving human subjects, thewater is not changed between smoking sessions. In our view, this entails a great bias which is seldom acknowledged (when the authors were aware of it) or even taken into account.
Hookah and Addiction
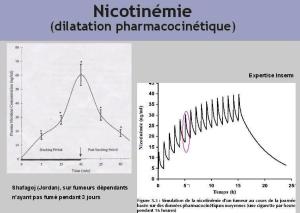
Dilating pharmacocinetics of nicotine in cigarettes smokers (right) and 3-day abstinent narghile dependent smokers (left)]. Source of the document: Chaouachi K. Cours sur le Narguilé. Université Paris XI 2007
For two decades now, the “Nicotine Addiction” model has been fatal for research in the field of cigarettes. Such a thesis is all the more irrelevant for the study of dependence among hookah smokers [9] .In Kuwait, a team has established with a rigorous methodology that the nicotine intake in hookah smokers is not as high as in cigarette users [18] . In Lebanon, researchers have found that more than 90% of so-called “mild smokers” (3 pipes or less per week) and about 50% of the so-called “moderate” ones (3 to 6 pipes per week) are considered as non dependent [2] . In this field, there is apparently no study on smokers of plain raw tobacco although early face-to-face interviews have been carried out and reported in a transdisciplinary doctoral thesis. In fact, nicotine in hookah smokers depends on a multitude of factors and situations. Some people can draw each day the nicotine equivalent of a pack-a-day cigarette smoker and others, perhaps the majority, might not absorb that of a single cigarette [5][11] . Even the official antismoking “”waterpipe”” experts who preparedthe WHO flawed report on ““waterpipe”” smokinghave recently found that the blood nicotine level, further to a 45 min hookah smoking session, did not reach that induced by a single cigarette [31] . Of course, and contrary to their claims, these results were established long before them by independent researchers, particularly in Egypt. Once again, hyping the risk of “nicotine addiction” among hookah smokers has nothing to do with the scientific method. The same goes for the “gateway” hypothesis (switching from hookah to cigarette smoking) put forward by antismoking researchers. It remains so far mere unsusbtantiated speculation . Please refer to the related sections (“Myth of Addiction“) in the SciTopics on the Global Epidemic and Mystique of Hookahs )
Hookah, ETS (Environmental Tobacco Smoke) & Charcoal Particles
 The following statement to be found in the WHO report (citing a study by the US-Syrian Centre for Tobacco Studies) is unsubstantiated: “Second-hand smoke from waterpipes […] poses a serious risk for non-smokers”[21][22] .Indeed, in striking contrast with cigarettes, hookah does generate almost no side-stream smoke [23] because of its peculiarities (charcoal topping the bowl and less elevated temperatures). So, the only smoke that should be taken into account is the one rejected by the smoker, i.e.the one filtered by the hookah at the level of the bowl, inside the water, along the hose and then by the smoker’s lungs themselves. 60 to 80% of the mainstream smoke particulate matter is retained in the lungs after inhalation” [24] . This last result, based on the review of studies covering one century, concerns cigarette smoke. It is even more relevant that hookah smoke is mainly made up of water and glycerol as in the Eclipse harm reduction cigarette. Consequently, the exhaled smoke is much less concentrated (in most of the toxic susbtances) than that of cigarettes. It is expected to be far less toxic for non-smokers than cigarette side-stream smoke [9][26][38] . Sadly enough, the issue of hookah ETS hazards is highly biased and the credibility of public health actions against the backdrop of a world epidemic has been stained because of a prohibitionist agenda (“smoke-free” cafes, homes, public gardens, cars, streets, entire cities, forests, etc.).In 2009, a 46 page study on this very issue was published in a peer-reviewed scientific journal [38] (table of contents available ). A shorter version was made available in another peer-reviewed medical journal [26] .
The following statement to be found in the WHO report (citing a study by the US-Syrian Centre for Tobacco Studies) is unsubstantiated: “Second-hand smoke from waterpipes […] poses a serious risk for non-smokers”[21][22] .Indeed, in striking contrast with cigarettes, hookah does generate almost no side-stream smoke [23] because of its peculiarities (charcoal topping the bowl and less elevated temperatures). So, the only smoke that should be taken into account is the one rejected by the smoker, i.e.the one filtered by the hookah at the level of the bowl, inside the water, along the hose and then by the smoker’s lungs themselves. 60 to 80% of the mainstream smoke particulate matter is retained in the lungs after inhalation” [24] . This last result, based on the review of studies covering one century, concerns cigarette smoke. It is even more relevant that hookah smoke is mainly made up of water and glycerol as in the Eclipse harm reduction cigarette. Consequently, the exhaled smoke is much less concentrated (in most of the toxic susbtances) than that of cigarettes. It is expected to be far less toxic for non-smokers than cigarette side-stream smoke [9][26][38] . Sadly enough, the issue of hookah ETS hazards is highly biased and the credibility of public health actions against the backdrop of a world epidemic has been stained because of a prohibitionist agenda (“smoke-free” cafes, homes, public gardens, cars, streets, entire cities, forests, etc.).In 2009, a 46 page study on this very issue was published in a peer-reviewed scientific journal [38] (table of contents available ). A shorter version was made available in another peer-reviewed medical journal [26] .
As a reaction to the latter, the US-American University of Beirut (now funded up to $ 3 million by the US National Cancer Institute in the wake of the above-mentioned pioneering study on cancer which came up with negative results) has immediately published an experimental study on side-stream smoke from hookahs. Its authors refer to an anonymous “controversy”(sic)…(i.e. our above mentioned publications…). The paper contains numerous errors and biases due, among others, to the use of a flawed smoking machine. Its main author (who also preparedthe WHO flawed report on ““waterpipe”” smokinga few years ago and who is a member of Globalink , the 6,000 member Pfizer-sponsoredworld antismoking network), has tried to justify the United Kingdom Ban on these grounds [36] . A critique was published in the same place [37] .
Finally, a German study was carried out in unrealistic conditions whereby 4 consecutive human smoking sessions of 40 min each took place in a non-ventilated room (the windows and the door were kept closed). Among other details, the water was not changed and the charcoal was still emitting bad particles… [1] . On one hand, this poses a very serious ethical problem wit h respect to protection of human subjects (Helsinki Declaration) [39] . On the other, the innocent “guinea pigs” had produced an “informed consent” (sic) in which they were not informed that they would be exposed to the dangerous chemical substances the researchers found (just to take one category of toxic chemicals): “concentrations of probable carcinogenic PAH during the session in indoor air which were 2.6 times higher than on the control day“. A critique has been published in the same journal (Food and Chemical Toxicology). It points out that “This figure being that of 4 consecutive smoking sessions, this means that even if such an experiment had been realistic, the concentrations for only one session prove to be even smaller than in the non-smoking condition…” [41] In their response, the authors say that during the 4-hour smoking session, there was actually “ventilation” as “fresh air could enter the room through the leaky [closed] windows” [42] … PS about political lobbying: Readers should keep in mind that independent research is permanently under attack and threats, particularly in the USA. Recently, a researcher from the University of Virginia, after drawing a review of pseudo-science (see discussion above), is waning local “public health” officials that “exemptions for hookah bars in clean indoor air legislation” is a “public health concern” [43] …See also a Knol about the made-in-the-USA Lebanese Smoking Ban .
h respect to protection of human subjects (Helsinki Declaration) [39] . On the other, the innocent “guinea pigs” had produced an “informed consent” (sic) in which they were not informed that they would be exposed to the dangerous chemical substances the researchers found (just to take one category of toxic chemicals): “concentrations of probable carcinogenic PAH during the session in indoor air which were 2.6 times higher than on the control day“. A critique has been published in the same journal (Food and Chemical Toxicology). It points out that “This figure being that of 4 consecutive smoking sessions, this means that even if such an experiment had been realistic, the concentrations for only one session prove to be even smaller than in the non-smoking condition…” [41] In their response, the authors say that during the 4-hour smoking session, there was actually “ventilation” as “fresh air could enter the room through the leaky [closed] windows” [42] … PS about political lobbying: Readers should keep in mind that independent research is permanently under attack and threats, particularly in the USA. Recently, a researcher from the University of Virginia, after drawing a review of pseudo-science (see discussion above), is waning local “public health” officials that “exemptions for hookah bars in clean indoor air legislation” is a “public health concern” [43] …See also a Knol about the made-in-the-USA Lebanese Smoking Ban .
[picture 1: WHO (World Health Organisation)-based photomontage (fake poster) by French INPES (Institut National pour la Prévention et l’Educationà la Santé), officially used in 2006 campaign against narghile and its “environmental tobacco smoke”]
[picture 2: Cigarette ETS (Environmental Tobacco Smoke) i s a mixture of aged diluted SSS (SideStream Smoke) (almost inexistent in hookahs) and EMSS (Exhaled MainStream Smoke). Credit: Formindep ]
Breath is Life…
As seen in the Diseases section, the main identified problems are, in case of medium to heavy use, respiratory complications in the long term.
If you are a hookah smoker and you wish to go on smoking despite all what you know about your practice, then avoid ill-ventilated venues and refrain from indulging in your habit more than one time a day for instance… If you wish to quit, for ever, hookah smoking, then avoid Nicotine “Replacement” Therapies (NRT) and associated products (patches, gums, etc.).You will spare a lot of money because these “aids” are not efficient and very expensive. Choose a more adapted method; one that targets desire, not nicotine… If you wish to quit hookah smoking but, for some reason, keep on on using tobacco, then think of harm reduction options like smokeless tobacco of the Swedish SNUS type [27] .
Other Online Resources
Qureshi Huma. Smoking shisha: how bad is it for you? It is growing in popularity but some experts say a single shisha session is the same as smoking 200 cigarettes. The Guardian (United Kingdom) 2011 (22 Aug)
Fahiemah Al-Ali & Connie Karambelas. Health effects of hookah, spot on or smoke and mirrors . Medill News Service 2010 (03 June)
Notes
This is a revised second draft. Please return for further hopefully updated and enriched versions.
Offer to National Public Health Authorities
All plans against the world hookah epidemic have failed. Time has come for an evaluation of the corresponding strategies that led to this negative outcome. It is only through open debate that science can progress. The author is ready to give advice on any relevant policies and healthy prevention programmes.
***********************************
REFERENCES [further to failed migration from the Knol articles]
1. Fromme H, Dietrich S, Heitmann D, Dressel H, Diemer J, Schulz T, Jörres RA, Berlin K, Völkel W. Indoor air contamination during a waterpipe (narghile) smoking session. Food Chem Toxicol. 2009 Jul;47(7):1636-41. http://dx.doi.org/10.1016/j.fct.2009.04.017 <http://dx.doi.org/10.1016/j.fct.2009.04.017>
2. Salameh P, Waked M, Aoun Z. Waterpipe smoking: Construction and validation of the Lebanon Waterpipe Dependence Scale (LWDS-11). Nicotine Tob Res. 2008 Jan;10(1):149-58
3. Millar N, Budgell BS. The language of public health—a corpus-based analysis. Journal of Public Health 2008;16: 369–74. http://www.lancs.ac.uk/postgrad/millarn/Files/Millar_Budgel_The%20language%20of%20public%20health.PDF <http://www.lancs.ac.uk/postgrad/millarn/Files/Millar_Budgel_The%20language%20of%20public%20health.PDF>
4. Chaouachi K. Harm Reduction Techniques for Hookah (shisha, narghile, “water pipe”) Smoking of Tobacco Based Products. Med Hypotheses 2009 Oct;73(4):623-4. http://dx.doi.org/10.1016/j.mehy.2009.06.016 <http://dx.doi.org/10.1016/j.mehy.2009.06.016>
5. Bacha ZA, Salameh P., Waked M. Saliva Cotinine and Exhaled Carbon Monoxide Levels in Natural Environment Waterpipe Smokers. Inhalation Toxicology 2007;19(9):771-7
6. Chaouachi K. Tout savoir sur le narguilé. Société, culture, histoire et santé. Paris [Eng.: Everything about Hookahs. Society, Culture, Origins and Health Aspects]. Maisonneuve et Larose 2007, 256 pages, colour. http://docs.google.com/View?docid=dgbz283m_19f97ts3 <http://docs.google.com/View?docid=dgbz283m_19f97ts3>
7. Chaouachi K. Narghilé: un problema di Sanità Pubblica [Public Health and Prevention]. Tabaccologia 2006;4. 29-38 http://www.tabaccologia.org/PDF/4_2006/7_42006.pdf <http://www.tabaccologia.org/PDF/4_2006/7_42006.pdf>
8. Van Der Merwe NJ: Cannabis Smoking in 13th-14th Century Ethiopia: Chemical Evidence. In World Anthropology: Cannabis and Culture. Edited by Vera Rubin: Mouton Publ. (The Hague); 1975: 77-80
9. Sajid KM, Chaouachi K, Mahmood R. Hookah smoking and cancer. Carcinoembryonic Antigen (CEA) levels in exclusive/ever hookah smokers. Harm Reduction Journal 2008 (24 May);5(19) http://www.harmreductionjournal.com/content/5/1/19 <http://www.harmreductionjournal.com/content/5/1/19>
10. Kozlowski, Kim. Michigan health leaders target growing hookah use. The Detroit News 2009 (14 Aug) http://detnews.com/article/20090814/LIFESTYLE03/908140351/1409/METRO/Mich.-health-leaders-target-growing-hookah-use <http://detnews.com/article/20090814/LIFESTYLE03/908140351/1409/METRO/Mich.-health-leaders-target-growing-hookah-use>
11. Chaouachi K. The Medical Consequences of Narghile (Hookah, Shisha) Use in the World. Revue d’Epidemiologie et de Sante Publique (Epidemiology and Public Health) 2007;55(3):165-70.[Article in English] Abstract <http://www.ncbi.nlm.nih.gov/pubmed/17446024>
12. Chaouachi K. Narghile (hookah, shisha) tobacco smoking: expect the unexpected everywhere and not only in Syria. Int J Infect Dis. 2009 Dec 15. [Epub ahead of print]. doi:10.1016/j.ijid.2009.08.016 http://dx.doi.org/10.1016/j.ijid.2009.08.016 <http://dx.doi.org/10.1016/j.ijid.2009.08.016>
13. Way, Tom. DiHydrogen Monoxide. DHMO Division 2009. http://www.dhmo.org/
14. [Comments on] Sajid KM, Chaouachi K, Mahmood R. Hookah smoking and cancer. Carcinoembryonic Antigen (CEA) levels in exclusive/ever hookah smokers. Harm Reduction Journal 2008 (24 May);5(19) http://www.harmreductionjournal.com/content/5/1/19/comments <http://www.harmreductionjournal.com/content/5/1/19/comments>
15. Chaouachi K. Public health intervention for narghile (hookah, shisha) use requires a radical critique of the related “standardised” smoking machine. Journal of Public Health [Springer Berlin/Heidelberg] 2009; 17(5): 355-xxx. DOI : 10.1007/s10389-009-0272-7 http://www.springerlink.com/content/58352477706011t0/ <http://www.springerlink.com/content/58352477706011t0/>
16. Al Rashidi M, Shihadeh A, Saliba NA. Volatile aldehydes in the mainstream smoke of the narghile waterpipe. Food Chem Toxicol. 2008 Nov;46(11):3546-9.
17. Meleigy M. Waterpipe and communicable diseases link, says WHO. The Lancet/Infections 2007 (July); Vol 7; issue 7:448 http://infection.thelancet.com <http://infection.thelancet.com>
18. Al-Mutairi SS, Shihab-Eldeen AA, Mojiminiyi OA, Anwar, AA. Comparative analysis of the effects of hubble-bubble (Sheesha) and cigarette smoking on respiratory and metabolic parameters in hubble-bubble and cigarette smokers. Respirology 2006; 11: 4…
19. Chaouachi K. Hookah (Narghile, Shisha) Smoking and Communicable Diseases. Tabaccologia 2008;1:47 [in English] http://www.tabaccologia.org/rivista.html <http://kamcha.googlepages.com/Hookah_Communicable_Diseases__Tabacc.pdf>
20. Chaouachi K. Micronuclei and Shisha/Goza Smoking in Egypt. Mutation Research/Genetic Toxicology and Environmental Mutagenesis 675 (2009) 81–82 Hard Consequences of Using the “”Waterpipe”” Scientific Nominalism <http://dx.doi.org/10.1016/j.mrgentox.2008.11.017>
21. Chaouachi K. A Critique of the WHO’s TobReg “Advisory Note” entitled: “Waterpipe Tobacco Smoking: Health Effects, Research Needs and Recommended Actions by Regulators” (2005). Journal of Negative Results in Biomedicine 2006 (17 Nov); 5:17 http://www.jnrbm.com/content/5/1/17 <http://www.jnrbm.com/content/5/1/17>
22. Maziak W, Ward KD, Afifi Soweid RA, Eissenberg T. Tobacco smoking using a waterpipe: a re-emerging strain in a global epidemic. Tobacco Control 2004; 13: 327-33
23. Deckers SK, Farley J, Heath J. Tobacco and its trendy alternatives: implications for pediatric nurses. Crit Care Nurs Clin North Am 2006 (Mar);18(1):95-104
24. Baker RR, Dixon M. The Retention of Tobacco Smoke Constituents in the Human Respiratory Tract. Inhalation Toxicology 2006; 17:255–94
25. Chaouachi K. Le Narguilé: Anthropologie d’un mode d’usage de drogues douces, Paris, L’Harmattan, 1997, 262 pages
26. Chaouachi K. Is Medical Concern about Hookah Environmental Tobacco Smoke Hazards Warranted ? The Open General & Internal Medicine Journal 2009; 3:31-3. http://www.bentham-open.org/pages/content.php?TOGMJ/2009/00000003/00000001/31TOGMJ.SGM <http://www.bentham-open.org/pages/content.php?TOGMJ/2009/00000003/00000001/31TOGMJ.SGM>
27. Rodu B, Phillips CV. Switching to smokeless tobacco as a smoking cessation method: evidence from the 2000 National Health Interview Survey. Harm Reduct J. 2008 May 23;5:18 http://www.harmreductionjournal.com/content/5/1/18 <http://www.harmreductionjournal.com/content/5/1/18>
28. Maziak W, Ward K, Eissenberg T. Interventions for waterpipe smoking cessation. Cochrane Database Syst Rev. 2007 Oct 17;(4):CD005549.
29. Sepetdjian E, Shihadeh A, Saliba NA. Measurement of 16 polycyclic aromatic hydrocarbons in narghile waterpipe tobacco smoke. Food Chem Toxicol 2008 May;46(5):1582-90 [BASED ON BIASED SMOKING MACHINE].
30. Chaouachi K. Prevention and sporadic carbon monoxide poisoning related to shisha (hookah, narghile) tobacco smoking. J Emerg Med. 2010 (Feb 2)[Epub ahead of print] . doi:10.1016/j.jemermed.2009.11.027 http://dx.doi.org/10.1016/j.jemermed.2009.11.027 <http://dx.doi.org/10.1016/j.jemermed.2009.11.027>
31. Eissenberg T, Shihadeh A. Waterpipe tobacco and cigarette smoking direct comparison of toxicant exposure. Am J Prev Med. 2009 Dec;37(6):518-23.
32. Chaouachi K. Hookah epidemic [Clarification about Cancer]. Br Dent J 2009; 207: 192-3. DOI: 10.1038/sj.bdj.2009.771 http://www.nature.com/doifinder/10.1038/sj.bdj.2009.771 <http://www.nature.com/doifinder/10.1038/sj.bdj.2009.771>
33. Ben Saad H. Le narguilé et ses effets sur la santé. Partie I : le narguilé, description générale et propriétés [The narghile and its effects on health. Part I: The narghile, general description and properties]. Rev Pneumol Clin 2009 65: 369 [Epub ahead of print 6 Nov]. Doi : 10.1016/j.pneumo.2009.08.010 http://www.ncbi.nlm.nih.gov/pubmed/19995660 <http://www.ncbi.nlm.nih.gov/pubmed/19995660>
34. Ben Saad H. Le narguilé et ses effets sur la santé. Partie II : les effets du narguilé sur la santé [The narghile and its effects on health. Part II: The effects of the narghile on health]. Rev Pneumol Clin 2009 [Epub ahead of print 6 Nov]. Doi : 10.1016/j.pneumo.2009.08.011 http://www.em-consulte.com/article/231124 <http://www.em-consulte.com/article/231124>
35. Video on the hazards of DiHydrogen Monoxide (DHMO) http://www.youtube.com/watch?v=yi3erdgVVTw <http://www.youtube.com/watch?v=yi3erdgVVTw>
36. Shihadeh A. [E-Letter] Findings on Waterpipe Second Hand Smoke. BMJ 2009 (20 Oct) http://www.bmj.com/cgi/eletters/335/7609/20#223088 <http://www.bmj.com/cgi/eletters/335/7609/20#223088>
37. Chaouachi K. Re: Findings on Waterpipe Second Hand Smoke. BMJ 2009 (11 Nov) http://www.bmj.com/cgi/eletters/335/7609/20#224837 <http://www.bmj.com/cgi/eletters/335/7609/20#224837>
38. Chaouachi K. Hookah (Shisha, Narghile) Smoking and Environmental Tobacco Smoke (ETS). A Critical Review of the Relevant Literature and the Public Health Consequences. International Journal of Environmental Research and Public Health. 2009; 6(2):798-843. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pubmed&pubmedid=19440416 <http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pubmed&pubmedid=19440416>
39. WMA (World Medical Association). Ethical Principles for Medical Research Involving Human Subjects. Adopted by WMA GA 18th GA (General Assembly), Helsinki (Finland), June 1964. Further amended until the 52nd WMA GA (Edinburgh, Scotland, Oct 2000). Clarification on Paragraph 29 added by WMA GA (Washington, 2002) and other on Paragraph 30 by WMA GA (Tokyo, 2004) http://www.wma.net/e/policy/b3.htm <http://www.wma.net/e/policy/b3.htm>
40. Cobb C, Ward KD, Maziak W, Shihadeh AL, Eissenberg T. Waterpipe tobacco smoking: an emerging health crisis in the United States. Am J Health Behav. 2010 May-Jun;34(3):275-85. http://www.ncbi.nlm.nih.gov/pubmed/20001185 <http://www.ncbi.nlm.nih.gov/pubmed/20001185>
41. Chaouachi K. Hookah (shisha, narghile, “water pipe”) indoor air contamination in German unrealistic experiment. Serious methodological bias and ethical concern. Food Chem Toxicol. 2010 Jan 25. [Epub ahead of print][UNCORRECTED proof]. Doi:10.1016/j.fct.2010.01.020 http://dx.doi.org/10.1016/j.fct.2010.01.020 <http://dx.doi.org/10.1016/j.fct.2010.01.020>
42. Fromme H. Response to comment on “indoor air contamination during a waterpipe (narghile) smoking session”. Food Chem Toxicol. 2010 Jan 25. [Epub ahead of print] http://www.ncbi.nlm.nih.gov/pubmed/20109514 <http://www.ncbi.nlm.nih.gov/pubmed/20109514>
43. Noonan D. Exemptions for hookah bars in clean indoor air legislation: a public health concern. Public Health Nurs. 2010 Jan-Feb;27(1):49-53. http://www.ncbi.nlm.nih.gov/pubmed/20055968 <http://www.ncbi.nlm.nih.gov/pubmed/20055968>
44. Nafae A, Misra SP, Dhar SN, Shah SN. Bronchogenic carcinoma in Kashmir Valley. Indian J Chest Dis. 1973 Oct; 15(4):285-95.
45. Rastam S, Li FM, Fouad FM, Kamal HM, Akil N, Moustafa AE. Water pipe smoking and human oral cancers. 1. Med Hypotheses. 2009 Nov 3. [Epub ahead of print] http://www.ncbi.nlm.nih.gov/pubmed/19892470 <http://www.ncbi.nlm.nih.gov/pubmed/19892470>
46. Fouad FM, Rastam S, Moustafa AE. Involvement of water pipe smoking in the development of human pancreatic cancer. Int J Cancer. 2009 Nov 23. [Epub ahead of print] http://www3.interscience.wiley.com/journal/123188924/abstract <http://www3.interscience.wiley.com/journal/123188924/abstract>
47. Prignot JJ, Sasco AJ, Poulet E, Gupta PC, Aditama TY. Alternative forms of tobacco use. Int J Tuberc Lung Dis. 2008 Jul;12(7):718-27.
48. Ray CS. The hookah – the Indian waterpipe. Current Science 2009; 96 (10):1319-23.
49. Chaouachi K, Sajid KM. A critique of recent hypotheses on oral (and lung) cancer induced by water pipe (hookah, shisha, narghile) tobacco smoking. Med Hypotheses 2009 (online: 24 Dec). Doi:10.1016/j.mehy.2009.11.036 http://www.ncbi.nlm.nih.gov/pubmed/20036075 <http://www.ncbi.nlm.nih.gov/pubmed/20036075>
50. Chaouachi K, Sajid KM. Cancer risks of hookah (shisha, narghile) tobacco use require further independent sound studies. Int J Cancer. 2010 Jan 20. [Epub ahead of print] http://www3.interscience.wiley.com/journal/123247817/abstract <http://www3.interscience.wiley.com/journal/123247817/abstract>
51. Ghasemi A, Syedmoradi L, Momenan AA, Zahediasl S, Azizi F. The influence of cigarette and qalyan (hookah) smoking on serum nitric oxide metabolite concentration. Scand J Clin Lab Invest. 2010 Feb 15. [Epub ahead of print] http://informahealthcare.com/doi/abs/10.3109/00365511003611282 <http://informahealthcare.com/doi/abs/10.3109/00365511003611282>
52. Akl E, Gaddam S, Gunukula SK, Honeine R, Abou Jaoude P, Irani J. The effects of waterpipe tobacco smoking on health outcomes: a systematic review. International Journal of Epidemiology. Advance Access published online on March 4, 2010. Doi:10.1093/ije/dyq002 http://ije.oxfordjournals.org/cgi/content/abstract/dyq002v1 <http://ije.oxfordjournals.org/cgi/content/abstract/dyq002v1>
53. Akl EA, Aleem S, Gunukula SK, Honeine R, Abou Jaoude P, Irani J. Survey instruments used in clinical and epidemiological research on waterpipe tobacco smoking: a systematic review. BMC Public Health. 2010 Jul 13;10(1):415. http://www.biomedcentral.com/1471-2458/10/415 <http://www.biomedcentral.com/1471-2458/10/415>
54. Raad D, Gaddam S, Schunemann HJ, Irani J, Abou Jaoude P, Honeine R, Akl EA. Effects of waterpipe tobacco smoking on lung function: a systematic review and meta-analysis. Chest. published 29 July 2010. Doi: 10.1378/chest.10-0991 http://www.ncbi.nlm.nih.gov/pubmed/20671057 <http://www.ncbi.nlm.nih.gov/pubmed/20671057>
55. Chaouachi K. [Peer-reviewed Comment] “Systematic Reviews” on ““Waterpipe”” (Shisha, Hookah, Narghile) Tobacco Smoking Should Not Recycle Old Errors. BMC Public Health 2010 (13 Aug) http://www.biomedcentral.com/1471-2458/10/415/comments <http://www.biomedcentral.com/1471-2458/10/415/comments>
56. Chaouachi K. Systematic Errors and Biases in “Systematic Review”on ““Waterpipe””:Source: “Peer-Reviewed” International Journal of Epidemiology. Knol. 2010 Aug 21 http://knol.google.com/k/kamal-chaouachi/systematic-errors-and-biases-in/534k6mvefph/17 <http://knol.google.com/k/kamal-chaouachi/systematic-errors-and-biases-in/534k6mvefph/17>
57. Khabour OF, Alsatari ES, Azab M, Alzoubi KH, Sadiq MF. Assessment of genotoxicity of waterpipe and cigarette smoking in lymphocytes using the sister-chromatid exchange assay: A comparative study. Environ Mol Mutagen. 2010 Aug 25. [Epub ahead of print]

Grant Cloete
Great Stuff — I guess it was a bad idea to quote the DHMO Vs Water joke in this article, especially since many would consider this article as important. Nevertheless, the points you bring across is very significant, although it won’t convince people that easily.I reckon you fight propaganda WITH propaganda. Don’t sit back and let the world swallow the lies the WHO are spreading across the internet.I mailed you a few mins ago, so please check your gmail account. I really want to clear up the confusion surrounding the dangers of smoking hookah.Anyway, keep up the good work. Soon when I get my engineering degree I’ll also be in a position to join the fight against those that publish experimentally proven lies.